Authors: Rami Bailony, MD, Sheryl Haller, Harun Yuksel, MD, Paulina Garzon, Roxanna Khalili, Imran M. Kyeso, Lydia Alexander, MD
Enara Health, San Mateo, CA, USA
Med-free and still mighty: 1 in 5 Enara patients lost over 15% of their weight—with no medications.
What made them different? Consistent, digital-first engagement.
Outcome: A digitally engaged population reached outcomes typically associated with surgery or AOMs.
Meet a 15% Club Member:
“I’d tried diets, gym memberships, even weight loss apps. What worked was accountability—having a team texting me, cheering me on, and helping me reset without judgment.”
Anonymous Enara patient, 36 months into program
Effective obesity care requires a multifaceted approach combining behavioral, lifestyle, pharmacologic, and surgical interventions. Recent studies highlight the potential of digital and remote engagement strategies in supporting weight maintenance. This study adds to the literature by evaluating the effectiveness of a comprehensive hybrid care model that combines traditional and digital elements.
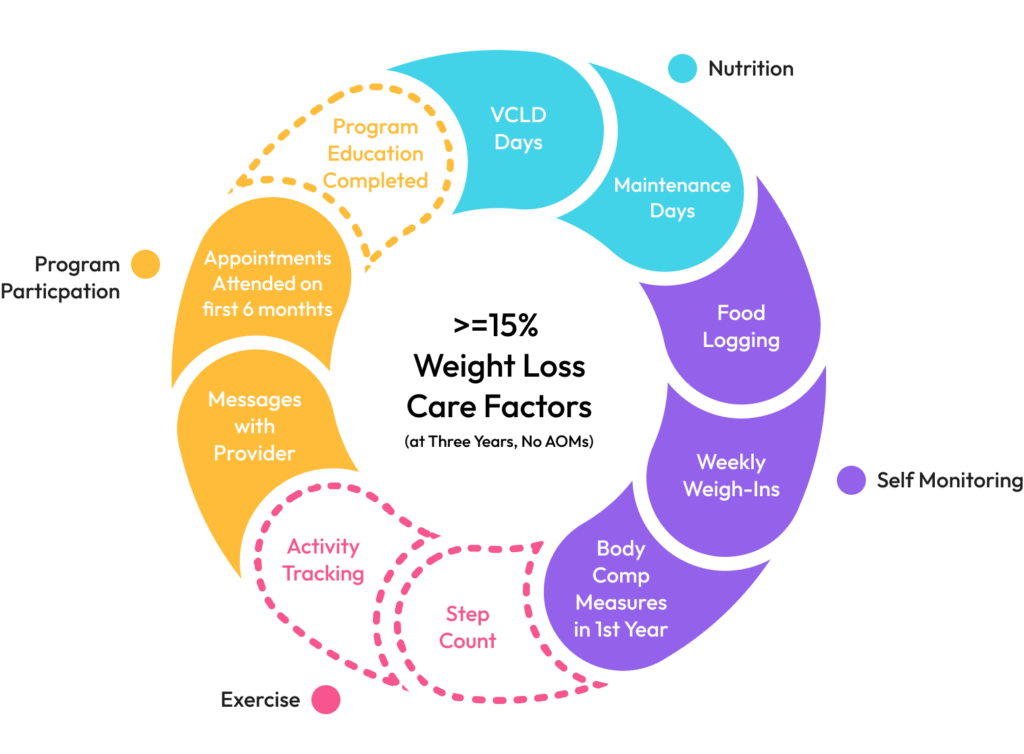
We conducted a retrospective study on adults who enrolled in a medical weight loss program and chose not to use anti-obesity medications (AOMs) over the first 36 months. High-performers were defined as participants who lost and maintained ≥15% of their starting weight. Factors evaluated included dietary approach, maintenance programming participation, monthly appointments, monthly provider text conversations, weekly food picture submissions, educational content completion, weekly weight monitoring, days using an activity tracker, and average monthly step count.
Out of 393 participants who did not use AOMs for 36 months, the average weight reduction was 8.93% ± 8.67. High achievers, representing 20.1% of participants, had significantly more monthly text conversations (17.81 vs. 15.25, p=0.04), food picture submissions (42.08 vs. 33.09, p<0.001), weekly weigh-ins (3.83 vs. 3.37, p=0.045), very low-calorie diet (VLCD) program days (120.10 vs. 77.54, p<0.001), and maintenance program days (375.27 vs. 225.10, p<0.001). There was no significant difference between high achievers and their counterparts in educational content completion, days using an activity tracker, or step count over 36 months. High achievement was linked to more frequent monthly appointments in the first 6 months (3.18 vs. 2.90, p=0.014) but not significant over 36 months.
Digital engagement components, such as text messaging, food logging, and weekly weight monitoring, were significantly associated with achieving and maintaining a 15% weight loss over 36 months. Traditional factors, including program type, maintenance participation, and appointment attendance but only in the first 6 months, were also associated with high achievement. Integrating remote digital engagement with traditional care elements enhances the effectiveness of obesity care programs, providing convenient tools for long-term weight management success.
Join 10+ cardiology practices already running Enara
Authors: M. Rami Bailony1, Hassan Kafri2 , Patricia Dizon3 ,University of California, San Francisco, CA; University of Damascus, Syria; University of Santo Tomas, Manila
Enara Health, San Mateo, CA, USA
Authors: Rami Bailony, MD, Imran M. Kyeso, Harun Yuksel, MD, Sheryl Haller, Lydia Alexander, MD.
Enara Health, San Mateo, CA, USA
Authors: Rami Bailony, MD, Imran M. Kyeso, Harun Yuksel, MD, Sheryl Haller, Lydia Alexander, MD.
Enara Health, San Mateo, CA, USA